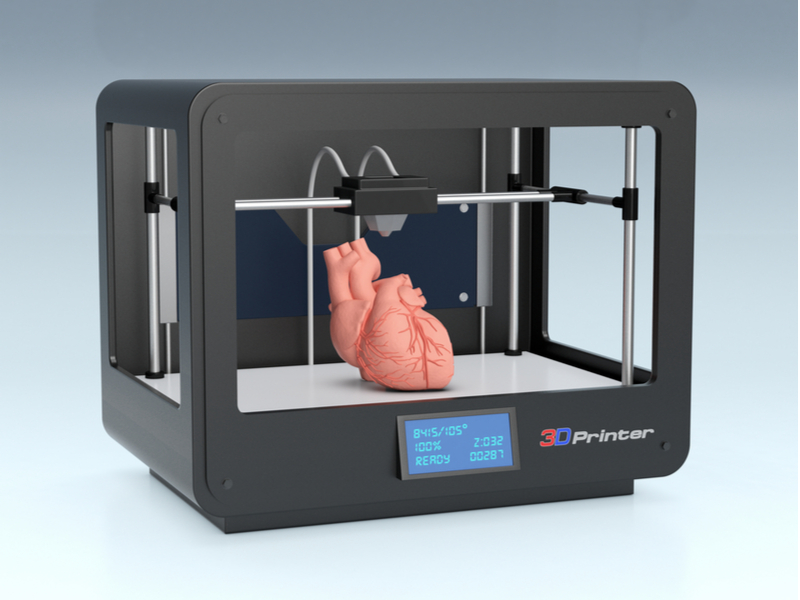
In the 21st century, 3D printing has emerged as a groundbreaking innovation. While many are still adapting to 2D printing, this advanced technology has rapidly expanded its capabilities, evolving from creating small toys to constructing massive buildings, and now, even bioprinting human organs for transplantation.
This remarkable progress promises a future where concerns over tissue damage, bone fractures, or heart failure could be significantly alleviated, offering new hope for patients.
The Revolution of 3D Bioprinting for Organ Transplants
The critical global shortage of transplantable organs leads to tragic outcomes, with many individuals succumbing before a suitable organ becomes available. For instance, in 2019, approximately 500,000 people in India alone died due to organ unavailability. To address this severe crisis and reduce extensive waiting lists, researchers have pioneered the 3D printing of biological organs, a revolutionary process known as ‘3D Bioprinting’.
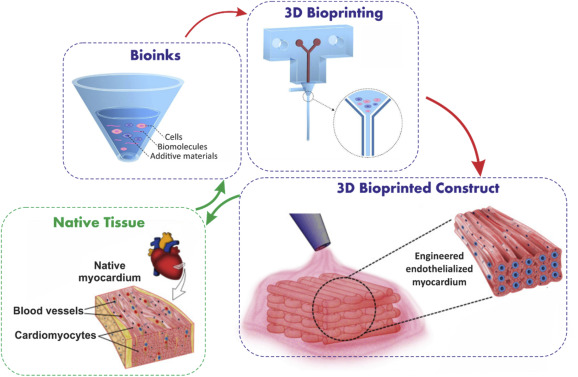
At its core, bioprinting involves the precise 3D printing of biomaterials—specialized substances used for biological fabrication—in successive layers to construct intricate bodily structures. This includes vital components such as skin, bones, corneas, and even complete hearts. A crucial aspect of successful organ transplantation is cellular compatibility. To mitigate rejection and enhance patient survival, the organs being bioprinted are engineered using the patient’s own cells. If patient-specific cells are not viable, adult stem cells can be utilized, which are then cultivated into a specialized ‘bioink’ to facilitate the printing process.
These nascent biological structures are meticulously held together and guided into their correct anatomical shapes by supportive elements like dissolvable gels or collagen scaffolds.
The ability to print functional body parts marks a significant leap forward in organ transplantation. By harvesting a transplant recipient’s own stem cells and bioprinting them into a replacement organ, this innovative approach can effectively circumvent common transplantation challenges, including prolonged waiting periods for compatible donors and the critical risk of immune rejection.
So, what specific organs have researchers successfully attempted to bioprint?
Breakthroughs in Bioprinting Bones
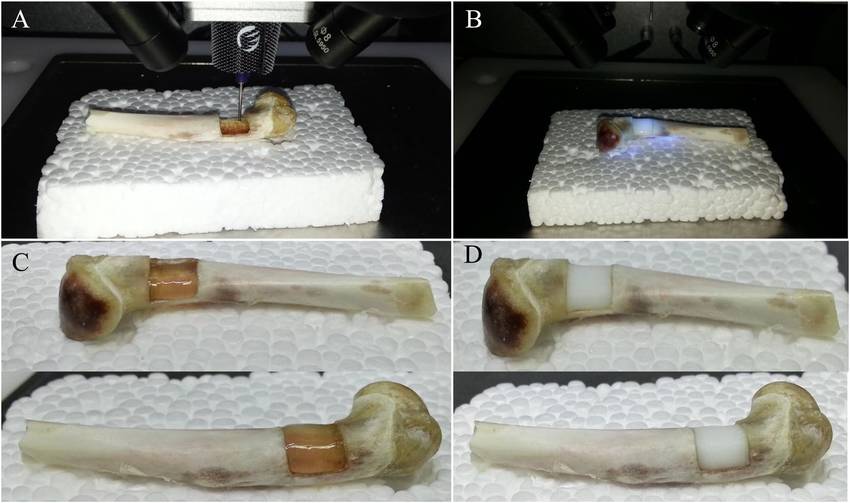
Innovators at Swansea University in the UK have successfully developed a bioprinting method for creating artificial bone matrix utilizing robust, regenerative biomaterials. Traditional treatments for severe bone fractures, such as ‘bone grafting’—involving the replacement of missing or damaged bone with synthetic or cement-based materials—often suffer from inadequate mechanical integrity and impede natural tissue formation.
In stark contrast, bioprinted bones offer a precise replica of missing bone structures, providing superior integrity, enhanced flexibility, and promoting natural tissue regeneration.
Innovations in Bioprinting a Human Heart

Researchers from the American Friends of Tel Aviv University have achieved a significant milestone by 3D printing a fully vascularized heart, using fat tissue cells sourced from a donor.
This groundbreaking process involved partially culturing the fat cells and then reprogramming them into functional heart cells. The resultant bioprinted heart showcased a complete anatomical structure, including all necessary cells, intricate blood vessels, ventricles, and chambers, meticulously designed based on medical imaging of the donor patient’s own heart.
While this technology represents a monumental step, it remains in its nascent stages. The bioprinted heart, currently the size of a rabbit’s heart, is not yet capable of pumping blood. Scientists are actively working on scaling up these organs and enabling them to beat rhythmically, with future plans to conduct animal testing.
Advanced Solutions for Tissue Regeneration
Annually, traumatic events such as vehicular accidents, workplace injuries, or acts of violence necessitate neurosurgical interventions for an estimated 22.6 million individuals, primarily due to significant tissue damage, particularly to nerves.
While conventional surgical techniques attempt to realign disconnected nerve ends and stimulate nerve growth, the outcomes are often inconsistent, with no guarantee of full functional restoration.
Read this: Selfie could be used to detect heart disease – AI study reveals
Leveraging 3D bioprinting, a dedicated research team successfully engineered a porous structure composed of the patient’s own neural cells combined with a biocompatible material to bridge an injured nerve. Alginate, a substance derived from algae, was specifically chosen for this application due to its excellent biocompatibility and minimal risk of rejection by the human body.
Although this promising technique has not yet undergone human trials, its refinement holds substantial potential to significantly benefit patients awaiting critical tissue and organ transplants.
Bioprinted Corneas: Restoring Vision
A historic moment in ophthalmology occurred on January 11 at Beilinson Hospital in Israel, where the world’s first synthetic cornea transplant was successfully performed. Following regulatory approval in 2020 to commence clinical trials for artificial synthetic cornea implantation, Israeli startup CorNeat Vision achieved a remarkable triumph by restoring the sight of a 78-year-old blind man who had suffered vision loss for a decade.
Innovating Skin Replacement with 3D Bioprinting
Replacing burned wounds with fresh skin is becoming more streamlined thanks to advanced 3D bioprinting techniques, offering a significant improvement over traditional skin grafting methods. Conventional grafting involves harvesting healthy skin from an unburnt area of the patient’s body, which becomes a limiting factor in cases of extensive burns. With bioprinting, a mere 10% of the burn area’s size is sufficient to yield enough cells for 3D printing new skin. The process begins with a specialized scanner determining the precise dimensions and depth of the wound. This data then guides the bioprinter to accurately deposit hypodermic, dermal, and epidermal skin cells at their respective depths, effectively covering the affected area.

As ongoing clinical trials and research progress, the team is keenly investigating the efficacy of stem cells derived from amniotic fluid and placentas, comparing their regenerative capabilities to those of patient-derived skin in facilitating wound healing.
Join our community by subscribing to our Weekly Newsletter to stay updated on the latest AI updates and technologies, including the tips and how-to guides. (Also, follow us on Instagram (@inner_detail) for more updates in your feed).
(For more such interesting informational, technology and innovation stuffs, keep reading The Inner Detail).